The Asian Journal of Neurosurgery has documented a case involving a rare tumour identified in a patient from Vadodara Gujarat.
The Neurosurgeon Dr. Vinay Rohra along with his teammates successfully removed a rare angiomyxofibromatous tumor from the falx cerebelli—marking what is believed to be the first documented case of its kind in the brain.
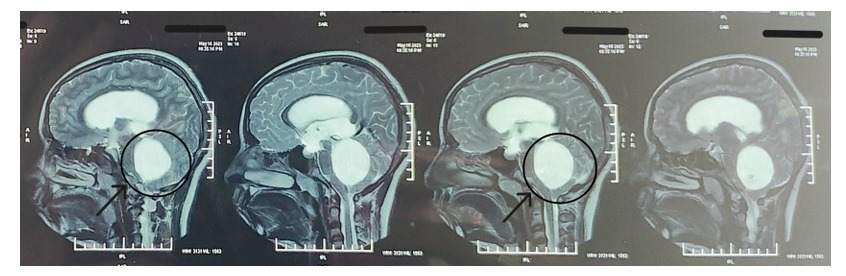
The lesion, which mimicked a fourth ventricular tumour on imaging, posed diagnostic and surgical challenges, ultimately leading to a milestone in medical literature.
The incident was published in Asian Journal of Neurosurgery on 26/05/2025.
A 13-year-old female patient presented with complaints of headache, dizziness, and blurring of vision for 3 months. Having no past medical history, the physical examination of the patient did not show any signs of Neurological deficits.
An MRI scan of the brain showed a clear, fluid-filled mass inside the fourth ventricle, a small space near the back of the brain. The mass was about 5 cm tall, 4 cm deep, and 4.3 cm wide—roughly the size of a golf ball. It appeared bright on the scan, which usually means it’s filled with fluid.
Myxoid tumours are a group of growths that doctors don’t yet fully understand or classify clearly. One type called myxoid glioneuronal tumor was officially recognized in 2021 by the World Health Organization. This tumour has certain unique features under the microscope, like special tumour cells surrounded by a jelly-like substance, sometimes with floating nerve cells inside.
This particular tumour is caused by a mutation in a gene called PDGFRA. However, the tumour in this case doesn’t fit into any known category or name doctors currently use.
However, in this case, the tumor wasn’t a pure myxoma because it had many blood vessels, so it was diagnosed as an Angiomyxofibromatous Tumor—a very rare tumour type. Only four cases of this tumour attached to a part of the brain called the falx cerebri have been reported before, and all were located above the brain’s tentorium (a membrane inside the skull).
This case was special because of where the tumour was located and how it showed up.
With the help of Immunohistochemistry, a special lab testing to identify proteins in tumor cells, doctors were able to understand this rare type of tumour better.
Based on previous reported cases, including this one, Angiomyxofibromatous tumors consistently test positive for a protein called vimentin, which suggests they come from mesenchymal (connective) tissue.
Some tumours also show positive results for S-100 protein and progesterone receptor (PGR), though this varies. Importantly, these tumours usually do not show markers found in brain or muscle tissue, such as GFAP (a brain cell marker), SMA (smooth muscle actin), cytokeratin (a skin and epithelial cell marker), and CD34 (a blood vessel marker).
However, one unique case reported by Sugita et al. showed additional findings—positivity for EMA (a membrane marker) and desman, which is typically found in muscle tissue—indicating that this tumour type may have some variation in its biological behaviour.
The patient was discharged in a week post operation and remains asymptomatic with no neurological deficits in follow up.
Despite the severity and rarity of the case, Dr. Vinay Rohra and the team of doctors were able to operate successfully, marking a significant medical achievement.